Do you notice your child sleeping with their mouth open?
Do they wake up tired even after a full night’s sleep?
Do they complain of morning headaches or seem irritable for no reason?
If you answered yes to any of these questions, you need to read this post all the way through.
As a pediatric dentist, I see this every single day: children who sleep poorly because of mouth breathing.
And as someone who was also a mouth breather during childhood due to recurring allergies, I know exactly how much this affects quality of life.
The good news? There’s a solution! And the sooner you act, the better.
Keep reading to understand what’s happening to your child and what you can do today to help them.
Child Mouth Breathing Sleep Problems: Understanding the Connection
Yes, there’s a direct relationship between mouth breathing and poor sleep quality.
Let me explain this simply.
When we breathe through our nose, the air is filtered, warmed, and humidified before reaching the lungs.
Additionally, nasal breathing activates receptors that help regulate deep sleep.
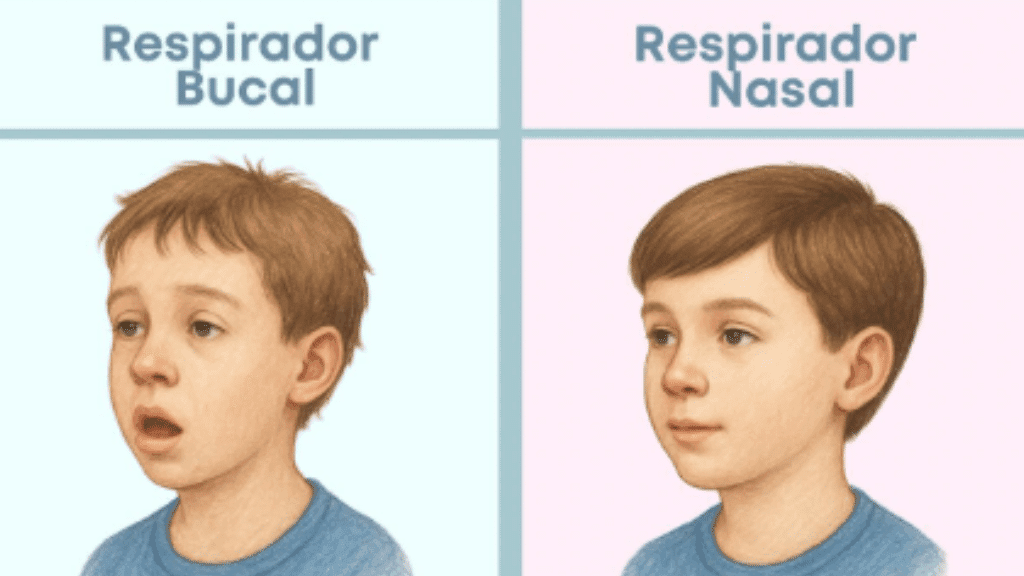
When a child breathes through their mouth:
The brain doesn’t receive enough oxygen during the night.
Sleep becomes fragmented and shallow.
The child wakes up multiple times without you noticing.
They can’t enter deep, restorative sleep.
The result?
Your child sleeps 10 hours but wakes up tired, irritable, and without energy.
It’s not laziness. It’s lack of quality sleep.
Why Does My Child Breathe Through Their Mouth While Sleeping?
This is the question every parent asks.
And there’s no single answer — each child has their own cause.
Let me show you the most common ones:
1. Nasal Obstruction
Enlarged adenoids are the number one cause.
These tissues at the back of the nose grow too large in some children (especially between ages 2 and 6).
They block the airway, forcing the child to breathe through their mouth.
Signs of enlarged adenoids:
- Frequent snoring
- Mouth always open, especially at night
- Nasal voice quality
- Recurring respiratory infections
Allergic rhinitis is also super common.
I had this myself as a child!
Chronically stuffy nose, constant sneezing, nose itching… sound familiar?
2. Enlarged Tonsils
Very enlarged tonsils make it difficult for air to pass.
The child “chooses” to breathe through their mouth to get enough oxygen.
3. Established Habit
Sometimes, even after resolving the nasal obstruction, the child continues breathing through their mouth.
It’s as if the brain “forgot” how to breathe through the nose.
This happened to me as a child. Even after treating the allergy, I needed to relearn how to breathe correctly.
4. Deviated Septum
Less common in young children, but it can happen.
Especially after some trauma to the nose.
5. Tongue Tie
A short lingual frenulum makes it difficult to position the tongue correctly.
This can favor mouth breathing.
The Dangers of Untreated Mouth Breathing
This is where my heart as a mother and my expertise as a dentist come together.
Untreated mouth breathing brings serious consequences.
Dental and Facial Problems
As a dentist, I see these problems every day:
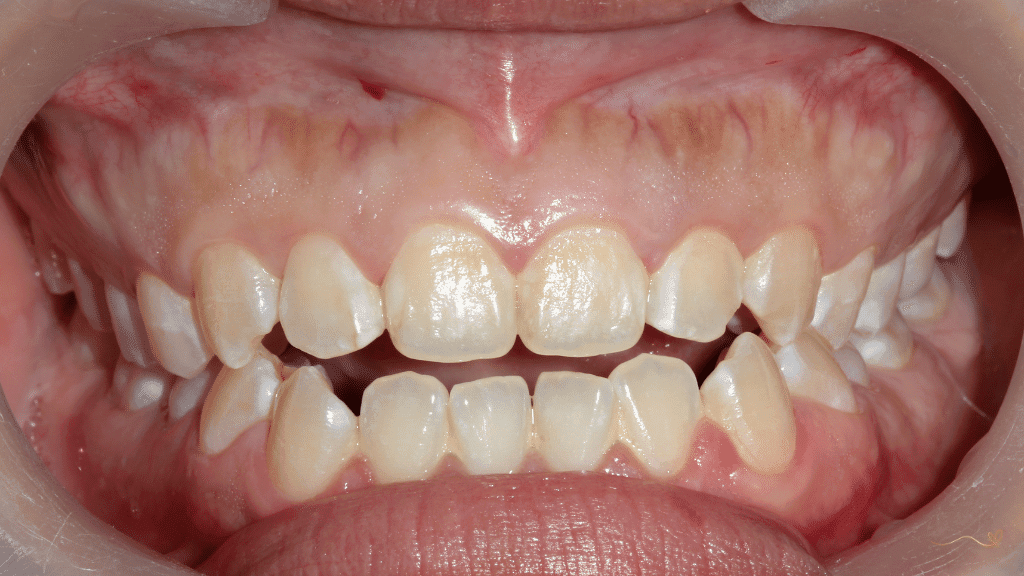
Malocclusion
The open mouth changes tongue position.
The tongue should rest on the roof of the mouth, but it stays down.
Without this natural pressure, the palate becomes narrow.
Teeth become misaligned and crowded.
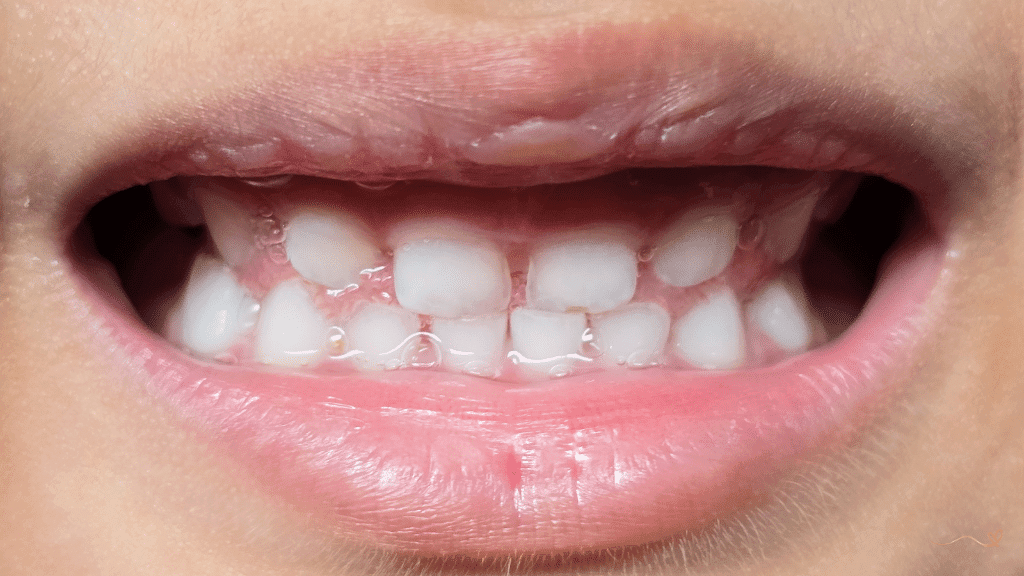
Open bite
The front teeth don’t touch when the child closes their mouth.
That space between upper and lower front teeth? That’s it.
Long face syndrome
Chronic mouth breathing changes facial growth.
The face becomes narrower and more elongated.
This is what we call “adenoid facies.”
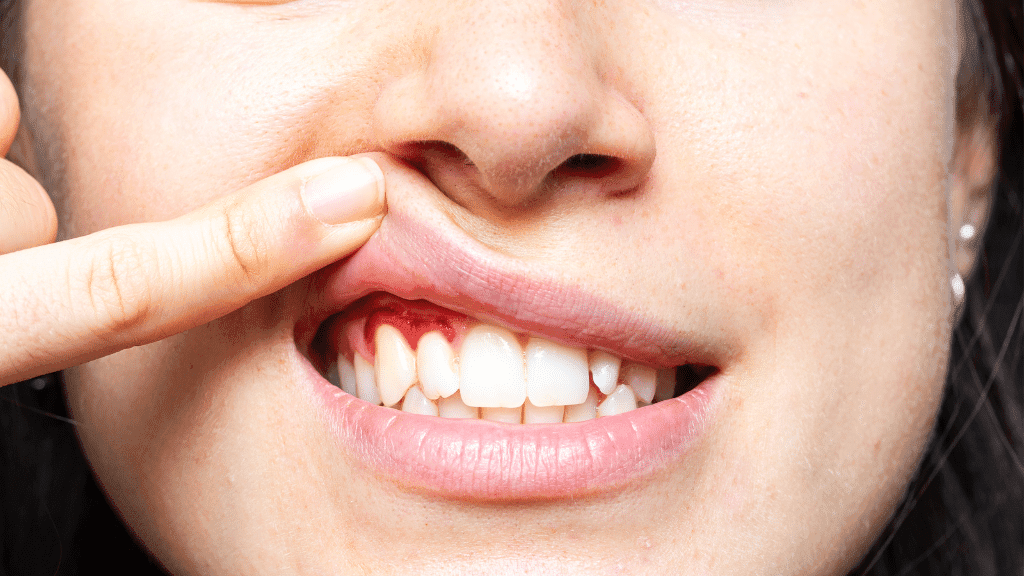
Gingivitis
The open mouth dries out the gums.
Dry gums become vulnerable to inflammation and bleeding.
Developmental Impacts
Difficulty concentrating
Children who sleep poorly have attention problems at school.
Often, what looks like ADHD is actually sleep deprivation.
Growth delay
Growth hormone is released during deep sleep.
Without this sleep, growth can be affected.
Behavioral changes
Irritability, frequent tantrums, easy crying.
Those difficult days? They might be related to poor sleep.
Low immunity
Mouth breathers get sick more frequently.
Air isn’t filtered by the nose, so viruses and bacteria enter directly.
The good news: the earlier you identify and treat, the better the results!
Children’s bodies have an incredible capacity for recovery.
7 Warning Signs You Should Watch For
It’s not always obvious that mouth breathing is affecting sleep.
Pay attention to these signs:
1. Frequent snoring (even if quiet)
2. Mouth open while sleeping (especially in the second half of the night)
3. Excessive drooling on the pillow
4. Restless sleep with many position changes
5. Waking up tired even after sleeping enough
6. Daytime sleepiness or difficulty waking in the morning
7. Dark circles or sunken eyes
If you checked 3 or more items, it’s time to investigate!
7 Practical Solutions to Help Your Child
Now comes the part you’ve been waiting for: what to do to solve it.
1. See an ENT Doctor
This is the first and most important step.
The ENT will examine adenoids, tonsils, and identify nasal obstructions.
Important: in most cases, it can be resolved without surgery!
Take your child to an ENT before age 5 if possible.
The earlier the diagnosis, the better the prognosis.
2. Treat Respiratory Allergies
If the problem is allergic rhinitis (like my case):
Eliminate dust mites from the bedroom with anti-allergen covers on mattress and pillow.
Avoid stuffed animals in bed.
Use an air purifier if possible.
Follow the treatment prescribed by the doctor rigorously.
My experience: when I finally treated my rhinitis properly, it was transformative!
3. Wash the Nose Daily
Saline solution is your best friend!
Wash your child’s nose:
- Upon waking
- Before bedtime
- Whenever it’s stuffy
How to do it:
Use a syringe (without needle) or nasal spray.
With the child’s head tilted to the side, apply saline in one nostril.
It will come out the other, cleaning the whole passage.
4. Elevate the Head of the Bed
Place a wedge under the mattress at the head end.
Elevate about 15 degrees.
This facilitates nasal drainage and reduces reflux.
Attention: DO NOT use extra pillows for babies under 1 year!
5. Humidify the Environment
Dry air worsens nasal obstruction.
Use a humidifier in the bedroom, especially in winter.
Important tip: clean the humidifier weekly to prevent mold!
6. Nasal Breathing Exercises
Turn it into a game!
Activities that help:
- Blowing bubbles (forces nose breathing)
- Blowing a whistle or horn
- Playing “who can hold their breath longest”
- Breathing deeply through nose and exhaling slowly through mouth
7. Speech Therapy
If mouth breathing has become a habit, a speech therapist can help.
Myofunctional therapy teaches the child to breathe correctly with specific exercises.
This re-educates the oral muscles.
When Is Surgery Necessary?
This is a frequent question in my office.
And I understand your concern as parents.
Adenoid surgery is indicated when:
Adenoids obstruct more than 70% of the airway.
The child has sleep apnea (stops breathing for seconds).
There are recurring ear infections.
Clinical treatment didn’t work after 6 months.
About the surgery:
It’s a simple and quick procedure (20-30 minutes).
Recovery is smooth in most cases.
Results appear almost immediately.
Many mothers tell me it was the best decision they made.
Why You Should Act Quickly
The first years of life are crucial.
This is when facial, dental, and brain development happens.
Problems not treated in childhood may require complex treatments later.
In my practice, I see cases of teenagers who need:
Orthodontic braces for years.
Palatal expander.
Sometimes even orthognathic surgery.
All of this could have been prevented with early treatment of mouth breathing.
You’re not overreacting by being concerned.
You’re being an attentive and caring parent!
My Personal Story as a Former Mouth Breather
Let me share something personal with you.
I was a mouth breather during childhood.
I had recurring allergic episodes that kept my nose constantly stuffy.
I slept poorly, woke up tired, had trouble concentrating at school.
My parents noticed and took action.
They took me to the doctor, we did proper allergy treatment.
But even after resolving the nasal obstruction, I continued breathing through my mouth.
It became a habit, you know?
I needed therapy with a speech therapist to relearn how to breathe through my nose.
Was it hard work? Yes.
Was it worth it? Every single second!
And as a dentist today, I see daily the consequences of untreated mouth breathing.
I see children at 10, 12 years old with serious dental problems.
Narrow palate, crowded teeth, open bite.
And I always think: “If they had been treated at 3, 4 years old…”
That’s why I insist so much: don’t wait!
Mouth Breathing and Teeth: What You Need to Know
Now I’ll talk specifically about the impacts on dentition.
The Tongue as a “Natural Appliance”
When a child breathes correctly through the nose, the tongue rests on the roof of the mouth.
This gentle, constant pressure molds the palate.
It makes it wide, with space for teeth to come in aligned.
But when breathing through the mouth:
The tongue stays down.
Without pressure on the roof of the mouth, the palate becomes narrow.
V-shaped instead of U-shaped.
Teeth become crowded and crooked.
Can develop crossbite.
Timing is Crucial
If you correct mouth breathing before ages 5-6, there’s a great chance of natural reversal.
The palate can still develop normally.
Teeth can come in more aligned.
If you wait until ages 10-12:
Will probably need a palatal expander.
Orthodontic braces for 2-3 years or more.
Sometimes even surgery.
Bottom line: treating now can save years of braces in the future!
Practical Tips for Daily Life
Here are tips that work and you can start today:
Sleep routine:
Wash nose 30 minutes before bedtime.
Avoid very cold air conditioning (dries the nose).
Leave a humidifier running in the bedroom.
Place a damp towel near the bed to help with humidity.
During the day:
Encourage games that require nasal breathing.
Avoid highly processed foods (increase mucus).
Keep the child well hydrated (water helps thin secretions).
Observation:
Take pictures of your child sleeping in profile once a week.
Note if they snore, drool, or wake up tired.
Bring this information to the doctor — it will help a lot with diagnosis!
Conclusion: Your Child’s Sleep Deserves Attention
If you made it this far, congratulations!
You’ve already taken an important step to improve your child’s life.
Let’s recap:
Mouth breathing during sleep prevents the child from resting properly.
It affects growth, behavior, dental development, and learning.
The most common causes are treatable: adenoids, tonsils, allergic rhinitis.
You can start today with simple measures.
But most importantly:
See an ENT specialist.
See a pediatric dentist specialized in mouth breathing.
Together, you’ll create the best plan for your little one.
Remember:
Each night of poor sleep is a missed opportunity for development.
But the good news is you have the power to change this!
I know because I lived it. My parents acted, I improved, and today I help other families.
Your turn to act has come.
If you have questions or want to share your experience, leave a comment!
Let’s talk, exchange ideas, support each other.
Warm regards,
Dr. Camila – Mommy Smile
Can I help you with anything else?
If you still have any questions, would like to leave a suggestion, or even share a concern, feel free to comment below or send me an email with love.
[email protected]
I personally read and reply to every message with care and attention
Frequently Asked Questions (FAQ)
1. At what age should I worry if my child breathes through their mouth?
From ages 2-3, you can identify chronic mouth breathing. If your child constantly breathes through their mouth (especially while sleeping) after this age, it’s worth investigating. Babies under 6 months may occasionally breathe through their mouth and it’s normal, but if it’s frequent, consult the pediatrician.
2. Can mouth breathing be cured?
Yes! In most cases, it can be completely cured. Treatment depends on the cause: it might be adenoid surgery, allergy treatment, speech therapy, or a combination. The earlier you treat, the better the results. I myself was a mouth breather and completely reversed it!
3. My child only breathes through their mouth when sleeping. Should I worry?
Yes, you should investigate. It’s during sleep that mouth breathing causes the most damage, as it prevents deep, restorative sleep. Even if they breathe through their nose during the day, if their mouth is open at night, it’s a sign of nasal obstruction or a habit that needs correcting.
4. Do pacifiers or bottles cause mouth breathing?
Not directly, but prolonged use (after age 3) can alter tooth and tongue positioning, favoring mouth breathing. Ideally, remove pacifiers and bottles by ages 2-3 to prevent oral development problems.
5. Can mouth breathing cause bad breath in children?
Yes! The open mouth dries out saliva, which is responsible for naturally cleaning the mouth. Without enough saliva, bacteria proliferate and cause bad breath. If your child has bad breath even when brushing well, it might be mouth breathing.
6. Does every mouth breather need surgery?
No! Many cases are resolved with clinical treatment: nasal washing, allergy treatment, speech therapy. Surgery is only indicated when there’s severe obstruction that doesn’t respond to conservative treatment. The doctor will evaluate each case individually.
7. Which specialist should I see first?
Start with an ENT (Ear, Nose, and Throat) doctor, who will evaluate adenoids, tonsils, and airways. In parallel, take your child to a pediatric dentist to assess impacts on dentition. If necessary, they’ll recommend a speech therapist to complement treatment.
8. Do braces fix mouth breathing?
No! Braces correct the consequences (crooked teeth, narrow palate), but don’t treat the CAUSE of mouth breathing. You must first resolve the breathing problem, then if necessary, do orthodontics. Otherwise, the problem can return!
9. How long does it take for a child to return to nasal breathing?
It depends on the cause and treatment. After adenoid surgery, there’s usually significant improvement within 1-2 weeks. In cases of established habit with speech therapy, it can take 2-6 months of therapy to re-educate breathing.
10. Can mouth breathing return after being treated?
If the cause was corrected (adenoids removed, allergy controlled), it rarely returns. However, if it became a habit and respiratory re-education with speech therapy wasn’t done, the child may continue breathing through their mouth even without physical obstruction. That’s why myofunctional therapy is so important!
Have you already discovered Jóia da Mamãe?
A gentle space for names, motherhood, and self-love
Name meanings and heartfelt inspiration to help you choose with love
Content that embraces motherhood with care, warmth, and gentleness
Mamãe Sorriso and Jóia da Mamãe walk side by side:
information, care, and love throughout every stage of motherhood.
If you care for oral health with Mamãe Sorriso, you’ll fall in love with the universe of Jóia da Mamãe
Visit Jóia da MamãeInformation, care, and love for the whole family